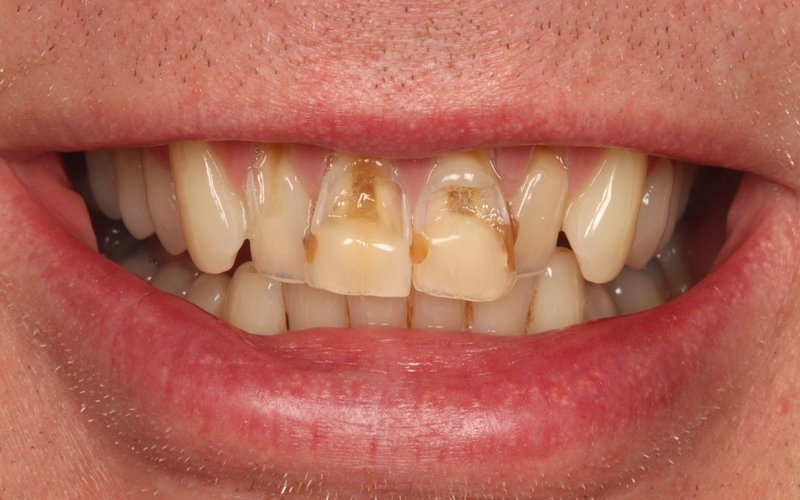
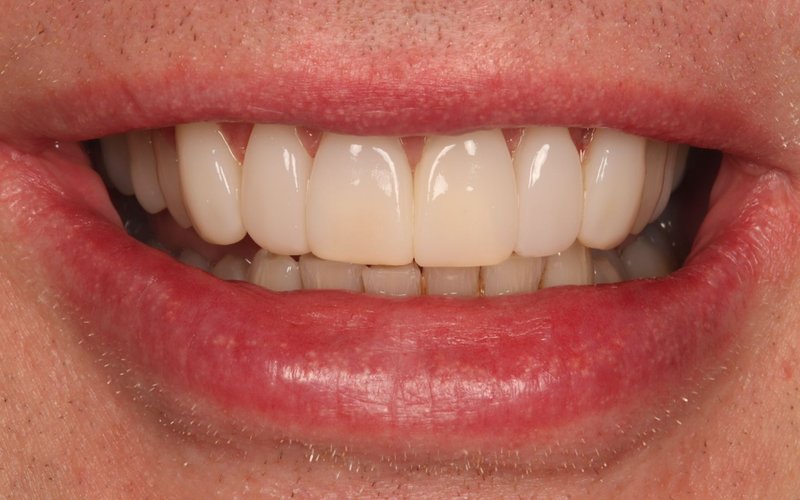
Dental Fillings in Blackpool — Natural, Long-Lasting Restorations at Tower Dental
Tower Dental Blackpool offers a full range of dental fillings to restore teeth affected by decay, chips, cracks or worn-down surfaces. Whether you require a simple composite filling or a more complex restoration, our GDC-registered team provide precision treatment in a calm, unhurried environment. We serve patients from across Blackpool, Cleveleys, Preston, Lytham St Annes and the wider Fylde Coast and Lancashire.
💬 Pricing is provided at your consultation — written quote, no obligation. Call 01253 353759 or book online.
At Tower Dental, we use tooth-coloured composite resin fillings as our material of choice for the vast majority of restorations. Unlike traditional amalgam (silver) fillings, white composite fillings are virtually invisible — they match the natural colour of your tooth so precisely that most people cannot tell a filling has been placed at all. They also require less removal of healthy tooth structure during preparation, helping to preserve more of your natural tooth.
Our principal dentist Dr Sarah Metias (MJDF RCS England, 19 years experience) and our experienced team take great care to ensure every filling is precisely shaped, correctly contoured and properly polished — restoring both the function and appearance of your tooth to the highest standard. If you are experiencing tooth pain or sensitivity that may indicate decay, call us immediately on 01253 353759 — early treatment prevents small problems becoming serious ones.
Dental Fillings at Tower Dental
Types of Dental Fillings Available at Tower Dental Blackpool (2026 Prices)
✅ White Composite Fillings
Our most popular choice. Tooth-coloured resin that bonds directly to your tooth — no mercury, minimal tooth removal, virtually invisible result. Ideal for front and back teeth.
🔄 Amalgam Replacement
Replace old silver/amalgam fillings with modern tooth-coloured composite. Improved aesthetics, no dark metal showing through enamel and eliminates concerns about mercury content.
🛡️ Composite Inlays & Onlays
For larger areas of decay or damage where a standard filling isn't sufficient but a full crown isn't yet needed. Custom-crafted to fit precisely and restore full biting strength.
🚨 Emergency Temporary Fillings
If a filling falls out or a tooth breaks, we provide same-day emergency temporary fillings to protect the tooth and relieve pain while a permanent solution is planned.
Signs You May Need a Filling
Not all decay causes immediate pain — in fact many cavities are often symptomless until they reach the nerve. Regular check-ups at Tower Dental allow us to identify decay early, before it causes discomfort or requires more extensive treatment. Signs that you may have a cavity and need a filling include:
- →Persistent toothache or sensitivity to hot, cold or sweet foods
- →A visible hole, pit or dark spot on a tooth
- →Pain when biting down on food
- →Food consistently getting stuck in a specific area
- →A rough or broken edge where a filling has cracked or fallen out
- →Grey or black discolouration on a tooth surface
The Filling Procedure — What to Expect
We assess the extent of decay using digital X-rays and confirm the best restoration option.
The area is completely numbed. You should feel no pain throughout — just pressure and vibration.
Decayed tooth material is carefully removed, preserving as much healthy tooth structure as possible.
Composite resin is layered, shaped and hardened. The filling is polished for a natural, smooth finish.
Why Replace Old Amalgam Fillings?
Many patients come to Tower Dental Blackpool specifically to have their old silver amalgam fillings replaced with modern white composite. There are several excellent reasons to consider this:
Aesthetics
Silver fillings can darken over time and cause the tooth to appear grey. White fillings match your natural tooth colour precisely.
Mercury-Free
Composite fillings contain no mercury. While amalgam fillings are considered safe, many patients prefer a mercury-free alternative.
Less Tooth Removal
Composite bonds directly to tooth structure, meaning less healthy tooth needs to be drilled away compared to amalgam preparation.
Longevity
Modern composite materials are highly durable. With proper care, white fillings typically last 7–12 years.
Dental Fillings in Blackpool — Serving the Fylde Coast
Tower Dental at 302a Devonshire Road, Blackpool FY2 0TW provides dental fillings to patients across Blackpool, Cleveleys, Fleetwood, Lytham St Annes, Poulton-le-Fylde, Kirkham, Preston, Garstang, Lancaster, Morecambe, Southport and throughout Lancashire. Free on-street parking is available directly outside the practice and a stairlift is provided for patients with limited mobility.
If you need a dental filling or suspect you may have a cavity, please don't delay — early treatment is always simpler, less expensive and more comfortable than waiting until pain develops. Call 01253 353759 or use our online booking form to arrange an appointment at Tower Dental Blackpool.
Dental Fillings Blackpool — FAQs
Related Treatments
Book Your Filling at Tower Dental Blackpool
302a Devonshire Road, Blackpool FY2 0TW · 01253 353759 · Same-day emergency appointments available
Explore More at Tower Dental Blackpool
Further Reading from Trusted UK Sources
For impartial, authoritative information on dental health, regulations and patient rights in the UK, the following organisations are recognised sources:
Authoritative UK sources on this topic
For independent, authoritative information from recognised UK health organisations:
External resources are provided for general education. Always consult a registered dental professional for advice specific to your circumstances.
Find Tower Dental Blackpool
302a Devonshire Road, Blackpool, Lancashire FY2 0TW · 01253 353759
"Composite (white) fillings are now the standard restorative material for most direct restorations in the UK, following the EU Minamata Regulation phase-out of mercury amalgam in deciduous teeth and high-risk groups."
Patient resources
Costs & feesTreatments & guides