Root Canal
Treatment in Blackpool
Root canal treatment is an endodontic procedure that removes infected or inflamed pulp tissue from inside a tooth, cleans and shapes the canal system and seals it with a biocompatible filling to save a tooth that would otherwise need extraction. It is indicated when there is irreversible pulpitis, a dental abscess, pain on biting that does not settle, or radiographic infection at the root tip. At Tower Dental Blackpool, root canal treatment is performed under local anaesthetic with rotary nickel-titanium instruments, magnification, rubber dam isolation and modern irrigation protocols by Dr Sarah Metias and Dr Alaaeldin Elraggal. Most cases are completed in one or two appointments of 60 to 90 minutes. A written quote is provided at consultation and a crown is usually recommended afterwards to protect the treated tooth. Where the tooth is unrestorable or has a vertical root fracture, extraction with implant replacement is the more predictable option.
Root Canal Treatment in Blackpool — Save Your Natural Tooth
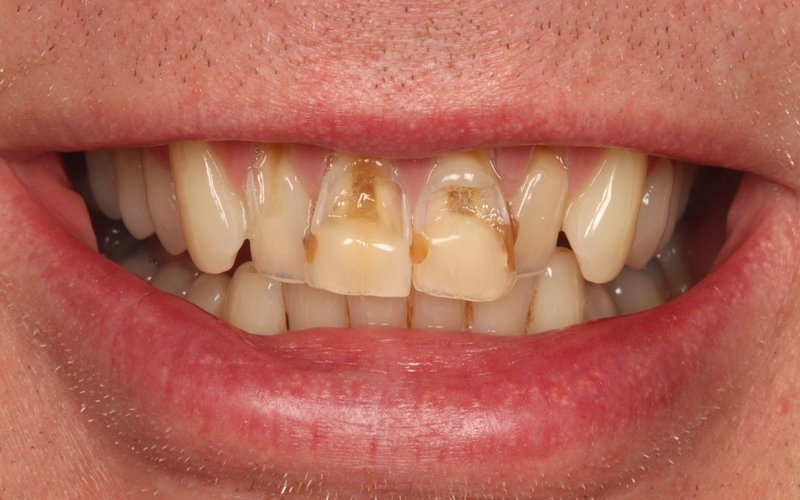
Root canal treatment in Blackpool at Tower Dental has an undeserved reputation for being painful. In reality, modern root canal treatment performed by our GDC-registered team is little different to having a filling — and it relieves the often intense pain caused by a dental infection. Root canal treatment at Tower Dental Blackpool allows us to save your natural tooth rather than extracting it, which is almost always the preferred option.
You may need root canal treatment in Blackpool if you have tooth pain, sensitivity to hot and cold, a dental abscess, or a damaged tooth with infected pulp. Tower Dental offers prompt appointments for root canal patients, including same-day emergency treatment where needed.
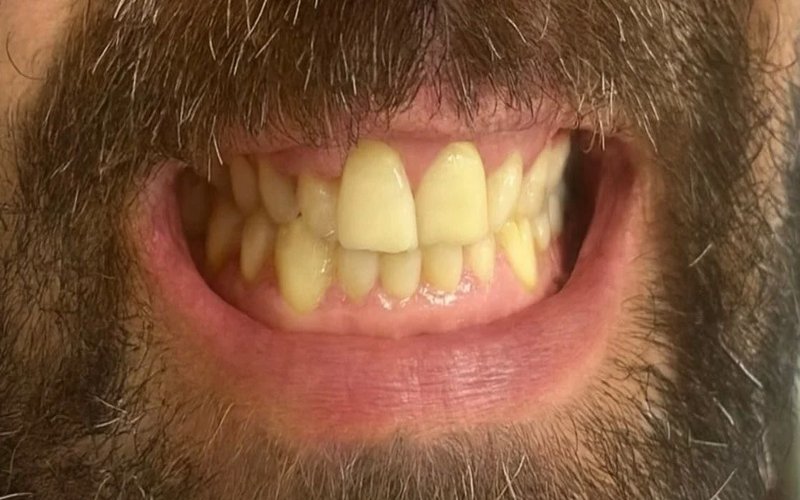
Severe toothache and infection requiring urgent treatment to save the tooth
Root Canal Treatment — Step by Step
Benefits of Root Canal Treatment
Root Canal Treatment Blackpool — FAQs
Ready to Get Started?
Book a consultation at Tower Dental Blackpool — 302a Devonshire Road FY2 0TW. Written quote, no obligation.
Root Canal Blackpool — Comfort-Focused Treatment at Tower Dental
Root canal treatment in Blackpool at Tower Dental has an undeserved reputation for being painful. In reality, our modern root canal in Blackpool is performed under local anaesthetic and is no more uncomfortable than a routine filling. Most patients are genuinely surprised by how comfortable the experience is. Root canal cost in Blackpool at Tower Dental — full written quote provided at consultation. 0% finance available.
💬 Pricing is provided at your consultation — written quote, no obligation. Call 01253 353759 or book online.
As a root canal dentist in Blackpool, Tower Dental offers same-day emergency root canal treatment for patients in acute pain. Our team includes Dr Safa Rafiq, who has a special interest in endodontics (the clinical field covering root canal treatment), ensuring patients receive expert endodontic care in a calm, reassuring environment. We treat root canal patients from across Blackpool, Cleveleys, Poulton, Fleetwood, Lytham St Annes, Preston and all FY postcodes.
If you are experiencing severe tooth pain in Blackpool that may require root canal treatment, do not delay. Call Tower Dental on 01253 353759 — we can usually see emergency patients the same day at our practice at 302a Devonshire Road, Blackpool FY2 0TW.
Explore More at Tower Dental Blackpool
Further Reading from Trusted UK Sources
For impartial, authoritative information on dental health, regulations and patient rights in the UK, the following organisations are recognised sources:
Authoritative UK sources on this topic
For independent, authoritative information from recognised UK health organisations:
External resources are provided for general education. Always consult a registered dental professional for advice specific to your circumstances.
Find Tower Dental Blackpool
302a Devonshire Road, Blackpool, Lancashire FY2 0TW · 01253 353759
"Endodontic treatment retains a tooth that would otherwise require extraction, with published 10-year tooth survival rates of 80-90% following primary root canal treatment in suitable cases."
Patient resources
Costs & feesTreatments & guides